
Get our Bad Breath Research Newsletter!
new!

2 phase
Mouthwash!
new!

2 phase
Mouthwash!
new!

2 phase
Mouthwash!



Originally appeared in Journal of
the American Dental Association 127:475-482, 1996. Used with permission.
Mel Rosenberg, Ph.D.
The Maurice and Gabriela Goldschleger School of Dental Medicine,
and the Department of Human Microbiology,
Sackler Faculty of Medicine,
Tel Aviv University,
Ramat Aviv 69978,
Israel
Telephone: 972-3-6429311
Fax: 972-3-6409250
Email: melros@post.tau.ac.il
Abstract
Bad breath is a common condition which usually originates in the mouth itself, and thus falls under the responsibility of the dental practitioner. In individuals with a healthy periodontium and good oral hygiene, bad breath usually comes from the posterior tongue dorsum, and can be treated by regular deep tongue cleaning. Nasal problems are an important secondary cause of bad breath, and are easy to detect by comparing the odor exiting the mouth and nose. Numerous other medical conditions can lead to bad breath, but are found very infrequently, as compared with odor of oral and nasal etiologies. Contrary to popular belief, the gastrointestinal tract is rarely, if ever, responsible for chronic bad breath. Because people have trouble assessing their own oral malodor, many individuals develop greatly exaggerated concerns of suffering from bad breath ("halitophobia"), while millions of others remain oblivious to their own oral odors. In most cases, good professional oral care combined with a daily regimen of oral hygiene including interdental cleaning, deep tongue cleaning and optional use of an efficacious mouthrinse, will lead to improvement. Cases in which the malodor continues to persist should be promptly referred to the physician.
The importance of bad breath to the dentist
Bad breath (oral malodor, halitosis) is a condition affecting tens of millions of
Americans. Although no one knows, it is likely that the  majority of the adult population suffers from
bad breath, at least occasionally.1 Since bad breath usually comes
from the mouth itself, the dentist should be the first professional that individuals turn
to.2 In the past, dentists have often circumvented patients' questions
regarding this problem. In recent years, however, there is a growing awareness that bad
breath is a problem which the dental professions should identify and address. Hundreds
(perhaps thousands) of US dentists currently advertise breath freshening as part of their
clinical services (M. Cohen, personal communication). Another reason why bad breath should
be of interest to dentists is that they may also suffer from this problem, to the chagrin
of family, staff and patients.2
majority of the adult population suffers from
bad breath, at least occasionally.1 Since bad breath usually comes
from the mouth itself, the dentist should be the first professional that individuals turn
to.2 In the past, dentists have often circumvented patients' questions
regarding this problem. In recent years, however, there is a growing awareness that bad
breath is a problem which the dental professions should identify and address. Hundreds
(perhaps thousands) of US dentists currently advertise breath freshening as part of their
clinical services (M. Cohen, personal communication). Another reason why bad breath should
be of interest to dentists is that they may also suffer from this problem, to the chagrin
of family, staff and patients.2
Together with the growing interest of dental practitioners in bad breath diagnosis and treatment, there has been a concomitant increase in research activity in this field, reflected in two recent international workshops dedicated solely to this subject.
The present review summarizes general concepts related to bad breath. Since the main clinical challenges for the practitioner are deciding (i) whether a given complaint of bad breath is justified; and (ii) whether the presenting odor originates in the mouth or elsewhere, emphasis has been placed on diagnostic modalities.
A short history
Bad breath has been with us for thousands of years. The problem is discussed at length in the Jewish Talmud3, as well as by Greek and Roman writers.4 Islam also stresses fresh breath in the context of good oral hygiene. The prophet Muhamed is said to have thrown a congregant from the mosque for having the smell of garlic on his breath.3 Ancient folk remedies abound which are still in use. The book of Genesis (Chapter 37) mentions ladanum (mastic), a resin derived from the Pistacia lentiscus tree (Figure 1) which has been used in Mediterranean countries for breath freshening for thousands of years. Other folk cures include parsley (Italy), cloves (Iraq), guava peels (Thailand) and eggshells (China).5
Modern literature on bad breath dates back to the monograph published by Howe in the nineteenth century6. Experimental research on the subject dates back over sixty years7,8. Since the 1960s the preeminent researcher in this field has been Dr. Joseph Tonzetich, at the University of British Columbia. Among other findings, Tonzetich and coworkers established that oral malodor is associated with the presence of volatile sulfur components, primarily hydrogen sulfide and methyl mercaptan (for a review, see reference 1).
The role of the oral cavity
In most cases (perhaps 85%), bad breath comes from the mouth itself1-3,6,8,9.
Various indications that bad breath originates in the mouth are listed in Table 1. The simplest way to distinguish oral from 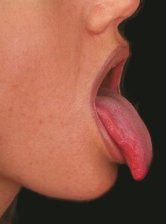 non-oral etiologies is to compare the smell
coming from the patient's mouth with that exiting the nose. If the odor is primarily from
the mouth, an oral origin may be inferred.7
non-oral etiologies is to compare the smell
coming from the patient's mouth with that exiting the nose. If the odor is primarily from
the mouth, an oral origin may be inferred.7
In people with rigorous oral hygiene, good dentition and a healthy periodontium, the main cause of bad breath is likely to be the back of the tongue.7,9 Although the anterior part of the tongue dorsum usually smells (a simple test is to lick one's wrist, waiting a few seconds until it dries out and then smell the area6), the main source of odor is usually further back in the posterior region7. The tongue dorsum posterior is most readily accessed by gentle but thorough scraping using a disposable plastic spoon.9 The spoon should be smelled and its odor compared to the overall mouth odor. In many cases, a yellowish discharge is collected on the spoon (Figure 2). Although there is no direct evidence, this discharge is probably postnasal drip9. Postnasal drip is extremely common, and is usually not indicative of any frank nasal infection or other pathology6. Although the postnasal drip might not smell initially when it first reaches the tongue (M. Littner and M. Rosenberg, unpublished observation), it can subsequently be putrefied by the abundant tongue microbiota. In subjects with periodontal disease, the tongue has been reported to be even more malodorous.11 Furthermore, the presence of three potential periodontopathogens (Treponema denticola, Porphyromonas gingivalis, and Bacteroides forsythus) on the tongue dorsum, as detected by the BANA™ test, was found to be significantly associated with the level of whole mouth odor in two studies.12,13 Odor from the posterior tongue dorsum may be present even in preschool children (R. Shimonov, D.M.D. thesis).
As with other body odors, bad breath is usually perpetrated by bacteria. Putrefaction is thought to occur under anaerobic conditions, involving a range of Gram-negative microorganisms, including species of Fusobacterium, Haemophilus, Veillonella, Treponema denticola, and Porphyromonas gingivalis.14,15 Although Gram-positive bacteria do not usually produce odor under laboratory conditions14, one research group has recently suggested (J. Greenman, M.A. El-Maaytah, M.G. Hartley and S. McAloon; Proteolytic activity of Stomatococcus mucilaginus; paper presented at 2nd International Workshop on Oral Malodor) that proteolysis by Gram-positive Stomatococcus mucilaginus contributes to subsequent tongue dorsum malodor.
Essentially any oral site in which microbial accumulation and putrefaction can occur are suspect.1 In addition to the most common intraoral sites of malodor production (the tongue, interdental and subgingival areas) other foci may include faulty restorations (e.g., overhangs, leaking crowns), sites of food impaction and abscesses. Caries are not considered to be particularly malodorous, unless sufficiently large to allow entrapment of food.2
 Dentures are
another important cause of oral malodor, particularly if they are worn overnight. Usually
the odor has a somewhat sweetish but unpleasant typical character and is readily
identifiable9, particularly if the dentures are placed in a plastic
bag and smelled following several minutes (Y. Kaufman and M. Rosenberg, unpublished
observation).
Dentures are
another important cause of oral malodor, particularly if they are worn overnight. Usually
the odor has a somewhat sweetish but unpleasant typical character and is readily
identifiable9, particularly if the dentures are placed in a plastic
bag and smelled following several minutes (Y. Kaufman and M. Rosenberg, unpublished
observation).
What role does saliva play in bad breath elaboration? In the individual, bad breath levels during the day are inversely related to saliva flow.16,17 When saliva flow is lowest (e.g., during the night, following fasting, due to insufficient water balance), bad breath rises. Conversely, mastication increases saliva flow, with concomitant cleansing of the oral cavity and reduction in malodor. 1,2,17 Despite these common observations, the data of two clinical studies did not support any association between saliva flow rate and malodor levels.18,19 Moreover, xerostomics do not appear to have higher-than-normal oral malodor levels (L. Sreebny, personal communication). Additional studies should be carried out to address this apparent paradox. One possible explanation for the latter observation is that malodor arises primarily in an alkaline microenvironment14, whereas the saliva of xerostomic patients is often acidic (L. Sreebny, unpublished data).
When in doubt concerning the oral etiology of the odor, the patient may be instructed to rinse and gargle for a week with a potent antibacterial mouthrinse (e.g., chlorhexidine-containing mouthrinses which have been shown in several studies18-20 to reduce odor levels significantly (p<0.001) for long periods following use). If malodor is significantly reduced, then an oral origin may be inferred.
Odor originating outside the mouth
Among nonoral etiologies of bad breath, the nasal passages predominate. In such cases, the telltale odor can be smelled most strongly from the nose, rather than the mouth. Nasal odor may be indicative of a frank nasal infection (such as sinusitis), or a problem affecting airflow or mucous secretions (e.g., polyps). In some cases, craniofacial anomalies, such as cleft palate, may be involved.10 The tendency of very young children to insert foreign bodies into their nostrils is a common cause of offensive odor that comes from the nose yet appears to emanate from the entire body.9 Typical nasal malodor usually has a slightly cheesy character and differs appreciably from other types of bad breath.9
The role of tonsils in chronic bad breath is not at all clear. The appearance of a transient odor during infections of the tonsils in children is common. Occasionally, tonsils emit a foul smelling exudate when pressed, although they appear normal upon visual examination10. In some individuals, the tonsillar crypts evolve concretions called tonsilloliths (Figure 3) which find their way onto the tongue. These stones are usually several millimeters in diameter, rough-edged, and white or yellowish. Although the stones themselves have a foul odor, particularly when pressed, they do not appear to be a significant source of bad breath9.
Many non-oral diseases, such as bronchial and lung infections, kidney failure, various carcinomas, metabolic dysfunctions, and biochemical disorders (for a summary, see reference 21) can result in bad breath, but all these taken together account for all only a very small percent of those suffering from the general problem. One interesting rare metabolic condition which leads to a perception of foul fishy odor and/or taste is trimethylaminuria.22 Whereas "acetone" breath was once considered a diagnostic indication for uncontrolled diabetes, very few cases are currently encountered (C. Hollenberg, personal communication).
Contrary to common thinking, bad breath from the gastrointestinal tract is considered to be extremely rare.2,7-9,23 The esophagus is normally collapsed and closed, and whereas the occasional belch may carry odor up from the stomach, the possibility of air escaping continously is remote.
Interestingly, for over a hundred years, people have smoked cigarettes in order to mask their bad breath7,22, a practice which results in an unattractive odor in its own right. Cigarette odor can linger for over a day following cessation of smoking. In some cases, one can detect the odor of cigarette smoke on the breath of subjects who do not smoke, but are continually exposed to the smoke of others (unpublished observations).
The bad breath paradox
Common experience teaches us that people are frequently unaware of their own bad breath2,3,8,9. Our inability to smell our own oral malodor has previously been attributed to adaptation, i.e., dulling of sensation due to continual exposure24.
We recently addressed this question in a study in which 52 subjects attempted to score the level of the malodor coming from their whole mouth, tongue dorsum and saliva.25 In the first two instances, subjects appeared completely unable to score their own smells in an objective fashion. In the case of saliva, some objectivity was evident. In all cases, subjects tended to score their own malodors according to preconceived notions. Based on the results of this study, it appears although the subjects had the physiological capability of smelling their own oral smells (shown by their semi-objective scoring of their own saliva malodor), their preconception of how bad their breath should smell confounded attempts at objectivity. Interestingly, in another study, self-estimates of bad breath by female subjects complaining of oral malodor were significantly higher than corresponding self-scores given by the male subjects (p<0.001), whereas actual odor judge scores revealed that the males had significantly higher levels of bad breath than the females (p<0.001).9
Whatever the underlying reasons, our insensitivity to our own bad breath can have grave consequences. People may spend their entire lives unaware that their breath is foul and offensive. Conversely, many others suffer from "halitophobia", i.e., a highly exaggerated fear that they suffer from bad breath.3 Halitophobics often practice social avoidance and are continually preoccupied with concealing the perceived odor (e.g., frequent toothbrushing, continuous gum chewing and candy sucking, keeping a safe distance, talking sideways).9 They are often secretive, and in many cases refrain from discussing the problem even with family members. During consultation, they often break into tears. One individual recently described the problem as a "nightmare". Another said that the fear of having bad breath "controls my soul". A third spoke of being "defiled".9 In extreme cases, halitophobics are driven to social isolation, may have their teeth extracted, and occasionally even commit suicide.11
What factors may predispose certain people to be overly concerned regarding bad breath? In some instances, patients may recall upon questioning that, as a child, someone in the immediate family (usually a parent) suffered from bad breath. Thus, the concern of having "inherited" this trait may crop up thirty years later. Advertisements on "jungle mouth" may elicit unwarranted concerns in suggestible individuals. Others may notice a bad taste in their mouth and assume (rightly or wrongly) that it must be related to bad breath. Some patients recall having been told once in their distant past that they had bad breath, yet have continued to worry about it ever since. Finally, as mentioned above, individuals with vile-smelling tonsilloliths may falsely infer that they have awful breath6.
Diagnosing bad breath in the dental clinic
Complaints of bad breath should be taken seriously by the dental practitioner, whether they appear justified or not.2 When a patient inquires in this regard it is important to set up a special appointment. Since individuals often clean or deoderize their mouths just before stepping into the dental clinic, the patient should be instructed to refrain from drinking, eating, chewing, rinsing, gargling, and smoking for at least two hours prior to the appointment. Patients should be asked to avoid using scented lipstick, aftershave and perfume on the day of the consultation. Malodor examinations should not be performed on patients taking antibiotics.2
The initial challenge is to determine whether the subject's complaint is well-founded, or has been blown out of proportion. Although history-taking can provide important clues (e.g., allergies, sinusitis, mouth breathing, polyps), self-reports of bad breath are notoriously subjective. For example, among 88 women presenting with a complaint of bad breath, 25 rated their own bad breath as "5" (the most foul odor imaginable) on a scale of 0-5, although corresponding judge scores ranged from 0 to 3.5.9 For this reason it is important to ask the patient to bring along a "confidant", usually a caring spouse or other family member. The confidant can usually provide a more objective picture of whether the patient actually suffers from bad breath, and to what extent. Since bad breath can vary with the time of day (e.g., as an inverse function of saliva flow) and day of the month (e.g., is sometimes worse during menstruation)26, the odor present at the consultation may or may not be similar to the odor at other times. The confidant can help determine whether the odor(s) present at the time of the consultation is typical, in quality and intensity, to the odor which is generally present.9
Instrumental analysis
Bad breath has previously been attributed to volatile sulphur components (VSC), primarily hydrogen sulfide and methyl mercaptan.1 The level of intraoral VSC can be estimated chairside, using portable sulfide monitors2. Several studies have shown that sulfide monitor readings are sensitive to reductions in mouth odor levels following use of efficacious mouthrinses17- 19. Associations comparing sulfide monitor results and odor judge scores are significant (coefficient correlations ranging from about 0.45 to 0.65, p<0.001 in various studies) and relatively reproducible.3 Incorporation of additional tests may further improve the association between sulfide monitor levels and odor judge scores. For example, in two studies, the association between volatile sulfur levels (as determined by the sulfide monitor) and odor judge scores was improved when BANA test results were factored into the regresion analysis.12,13 In a third investigation BANA scores were associated (p=0.001) with the odor obtained following proximal dental floss passage, and were reduced following chlorhexidine rinsing.19 Whereas such quantitative and semi-quantitative measurements can be of assistance (for example, when testing for improvement following treatment), they do not obviate the need for the clinician to actually smell the breath emanating from the mouth, nose and tongue of the patient.
In an influential study published in 1967,27 Tonzetich and coworkers argued that bad breath derives exclusively from sulfur-containing volatiles. They based this on the observation that other volatiles tested did not escape from the saliva into the air. However, Kleinberg and Codipilly14 have recently shown that when the skin dries out, non-sulfur containing gases, such as cadaverine, putrescine, skatole, indole, butyric acid and isovaleric acid can be released over time. Similarly, the malodor of an extract of putrefied saliva, placed on the skin, lingers for over two hours (unpublished observation). The implication is that when saliva dries out on oral surfaces, a range of VSC and other volatiles are released. This is in agreement with the observation that bad breath increases when the mouth is dry.16,17 Furthermore, results in our laboratory show correlations between salivary levels of cadaverine and oral malodors.28 Indeed, when sulfide monitor scores and salivary cadaverine levels are both taken into account, the correlation with odor judge scores increases significantly.28 Unfortunately, cadaverine is difficult to assess in the dental clinic. However, as mentioned above, BANA testing of samples obtained from various intraoral sites12,13,19 and perhaps other tests (e.g., the Oratest, which was the only test other than volatile sulfide levels to show significant associations with bad breath in children [R. Shimonov, D.M.D. thesis]) can be useful. Someday in the not-too-distant future, electronic "noses" which distinguish among different kinds of smells will be available for bad breath testing. Eventually, individuals may be able to breathe into their telephone mouthpiece and receive an on-line breath analysis!
Despite the advantages of the tests mentioned above, clinicians interested in diagnosing bad breath must still rely on their noses to distinguish the main types of oral odors (Table 2). These include (i) periodontal-type odor (all too familiar to practicing dentists) which usually comes from periodontal pockets and interdental spaces; (ii) odor from the posterior tongue dorsum (can easily be recognized by smelling the spoon following scraping); (iii) denture odor (readily smelled by placing the dentures into a plastic bag for several minutes); (iv) characteristic nasal odor (easily identified on the breath exiting the nose); and (v) smoker's breath. With practice and experience, these odors become distinct and recognizable, even when found in various combinations.
In some cases, although little odor appears on the breath when the patient breathes out through the mouth, the odor becomes apparent when the patient starts speaking (M. Rosenberg and E. Leib, unpublished observation). Thus, in addition to asking the subject to breathe out through mouth and nose, we now routinely ask the patient to count out loud to twenty, and smell the odor while the patient counts.

Treating bad breath in the dental clinic
The best way to treat bad breath is to instill patients with good oral hygiene practices and to ensure that their dentition is properly maintained.1,2 Although patients often balk at using dental floss, once the connection is made between flossing and fresh breath (e.g., just by asking the patients to smell their own floss following each passage), compliance improves.2 In one study, subjects who flossed were found to have significantly less mouth odor (p=0.016), saliva odor (p<0.001) and salivary cadaverine levels (p=0.011) than those who did not (D. Gordon, D.M.D. thesis). Furthermore, one year following the initial oral malodor examination, the percentage of subjects who flossed their teeth rose from 31% to 65% (Y. Wind, D.M.D. thesis). Other interdental cleaners (e.g. anatomic plastic toothpicks) can also be effective in identifying and cleaning sites of odor production.
Gentle but effective deep tongue cleaning should be an important daily routine. A variety of tongue scrapers have been produced in recent years (Figure 4). Cleaning the tongue can also be performed by brushing with any toothbrush that minimizes gagging reflex. In order to prevent tongue odor, the tongue should be brushed in a gentle, but thorough manner, keeping in mind that the posterior portion is the area which is the least accessible, yet smells the worst.7-9 Even patients with significant gagging reflex can get used to cleaning the back of their tongue with some practice.
Since bad breath is worse when the mouth dries out (e.g., at night, while fasting), subjects should be encouraged to maintain a good water balance. Chewing gum is also helpful in reducing bad breath during the day, although its use should be restricted to only a few minutes at a time, to avoid temperomandibular joint problems.2
Many people continue to have malodor of oral origin, even after carrying out oral hygiene practices. In such instances, rinsing and gargling with an efficacious mouthwash may be advised. It should be kept in mind, however, that many mouthwashes contain components which may have a non- beneficial effect on soft oral tissues (e.g., alcohol, sodium dodecyl sulfate, strong oxidizing agents). The best time to use a mouthwash is probably before bedtime, since (i) residue of the mouthrinse may remain in the mouth for a longer period of time and have a greater effect; and (ii) bacterial activity leading to bad breath is greatest during the nighttime, when saliva flow is practically zero and microbial activity is highest.1
Although there may be a dramatic reduction in an individual's bad breath following consultation and treatment, the patient may find it difficult to sense the improvement (A. Fleming, personal communication). This problem can be addressed with the help of the "confidant", who can help monitor changes over time. In those cases in which the odor (or the subjective complaint) persists, the patient should be promptly referred to the physician for further assessment.
Being frank about bad breath
Should a dentist tell a patient with bad breath that he/she suffers from the problem, even when the patient does not complain? This is an onerous, but important task. One possibility is to make an oblique, generalized comment about the connection between oral hygiene and bad breath. For example, the dental professional might ask "Did you know that people who don't floss their teeth daily may suffer from bad breath?". The patient might then ask "Are you implying that I have bad breath?" The dentist or hygienist could then respond "I suggest that you ask someone in your family, and then get back to me on it."
Certainly, it is difficult to tell patients, friends and associates that they suffer from this problem. However, at the very least, we should be prepared to tell the ones we love and care for if they suffer from bad breath, and to hope that, if necessary, they will reciprocate in kind.
Conclusions
Several of the central concepts in diagnosis and treatment of oral malodor are:
- Bad breath is a common condition which usually comes from the mouth itself, and rarely from the gastrointestinal tract.
- The dentist has the primary responsibility for diagnosing and treating bad breath.
- The posterior of the tongue dorsum posterior is the most frequently overlooked source of oral malodor. It can be readily sampled using a plastic spoon.
- Patients complaining of bad breath should be assigned a separate appointment, and should be encouraged to bring along a family member or close friend (confidant).
- Because of the difficulty inherent in smelling our own bad breath, many individuals harbor grossly exaggerated concerns while others remain unaware that they suffer from the problem.
- Although correlative quantitative measurement techniques are available and helpful, the clinician should also make a differential judgement based on actual smelling of the odor emanating from the patient's mouth and nose.
- In most cases, bad breath can be ameliorated by proper dental care, oral hygiene, deep tongue cleaning and, if necessary, rinsing with an effective mouthwash.
- If the problem persists (or the perception of suffering from the problem persists), the patient should be promptly referred for appropriate medical care.
- Tonzetich J. Production and origin of oral malodor: a review of mechanisms and methods of analysis. J Periodontol 1977;48:13-20.
- Rosenberg M. Bad breath: Diagnosis and treatment. U Toronto Dent J 1990;3:7-11.
- Rosenberg M. Introduction, in Bad Breath:Research Perspectives, Rosenberg M, ed, Ramot Publishing - Tel Aviv University (1995) pp 1-12.
- Geist H. Halitosis in ancient literature. Dent Abstr 1957;2:417-418.
- Rosenberg M. Diagnosis and treatment of bad breath. Cosm & Toil (in press).
- Howe JW. The breath and the diseases which give it a fetid odor. 4th ed., New York: D. Appleton and Co.;1898.
- Grapp GL. Fetor oris (halitosis). A medical and dental responsibility, Northwest Med 1933;32:375-80.
- Prinz H. Offensive breath, its causes and its prevention. Dent Cosmos 1930;72:700-707.
- Rosenberg M, Leib E. Experiences of an Israeli malodor clinic, Ch 9 in Bad Breath:Research Perspectives, M Rosenberg, ed, Ramot Publishing - Tel Aviv University (1995) pp 137-148.
- Finkelstein Y. The otolaryngologist and the patient with halitosis, Ch 11 in Bad Breath:Research Perspectives, M Rosenberg, ed, Ramot Publishing - Tel Aviv University (1995) pp 175-188.
- Yaegaki K. Oral malodor and periodontal disease, Ch 6 in Bad Breath:Research Perspectives, M Rosenberg, ed, Ramot Publishing - Tel Aviv University (1995) pp 87-108.
- De Boever EH, De Uzeda M, Loesche WJ. Relationship between volatile sulfur compounds, BANA-hydrolyzing bacteria and gingival health in patients with and without complaints of oral malodor. J Clin Dent 1994;4:114-119.
- Kozlovsky A, Gordon D, Gelernter I, Loesche WJ, Rosenberg M. Correlation between the BANA test and oral malodor parameters. J Dent Res 1994;73:1036-1042.
- Kleinberg I, Codipilly M. The biological basis of oral malodor formation, Ch 2 in Bad Breath:Research Perspectives, M Rosenberg, ed, Ramot Publishing - Tel Aviv University (1995) pp 13-39.
- Persson S, Claesson R, Carlsson J. The capacity of subgingival microbiotas to produce volatile sulfur compounds in human serum. Oral Microbiol Immunol 1989;4:169-172.
- Tonzetich J. Oral malodour: An indicator of health status and oral cleanliness. Int Dent J 1977;28:309-319.
- Rosenberg M, McCulloch C.A.G. Measurement of oral malodor: current methods and future prospects. J Periodontol 1992;63:776-782.
- Rosenberg M, Kulkarni GV, Bosy A, McCulloch CAG. Reproducibility and sensitivity of oral malodour measurements with a portable sulphide monitor. J Dent Res 1991;70:1436-.40.
- Bosy A, Kulkarni GV, Rosenberg M, McCulloch CAG. Relationship of oral malodor to periodontitis: evidence of independence in discrete subpopulations. J Periodontol 1994;65:37-46.
- Rosenberg M, Gelernter I, Barki M, Bar-Ness R. Daylong reduction of oral malodor by a two-phase oil:water mouthrinse, as compared to chlorhexidine and placebo rinses. J Periodontol 1992;63:39-43.
- Attia EL, Marshall KG. Halitosis. Can Med Assoc J 1982;126:1281-85.
- Preti G, Clark L, Cowart BJ, Feldman RS, Lowry LD, Weber E, Young I-M. Non-oral etiologies of oral malodor and altered chemosensation. J Periodontol 1992;63:790-796.
- Hawxhurst DC. Offensive breath. Dent Register 1873;27:104-110.
- Spouge JD. Halitosis: a review of its causes and treatment. Dent Practit 1964;14:307-317.
- Rosenberg M, Kozlovsky A, Gelernter I, Cherniak O, Gabbay J, Baht R, Eli I. Self estimation of oral malodor. J Dent Res 1995;1577-1582.
- Tonzetich J, Preti G, Huggins GR. Changes in concentration of volatile sulphur compounds of mouth air during the menstrual cycle. J Int Med Res 1978;6:245-256.
- Tonzetich J, Eigen E, King WJ, Weiss S. Volatility as a factor in the inability of certain amines and indole to increase the odor of saliva. Arch Oral Biol 1967;12:1167-1175.
- Goldberg S, Kozlovsky A, Gordon D, Gelernter I, Sintov A, Rosenberg M. Cadaverine as a putative component of oral malodor. J Dent Res 1994;73:1168-1172.
Originally appeared in Journal of the American
Dental Association 127 :475-482, 1996. Used with permission.
